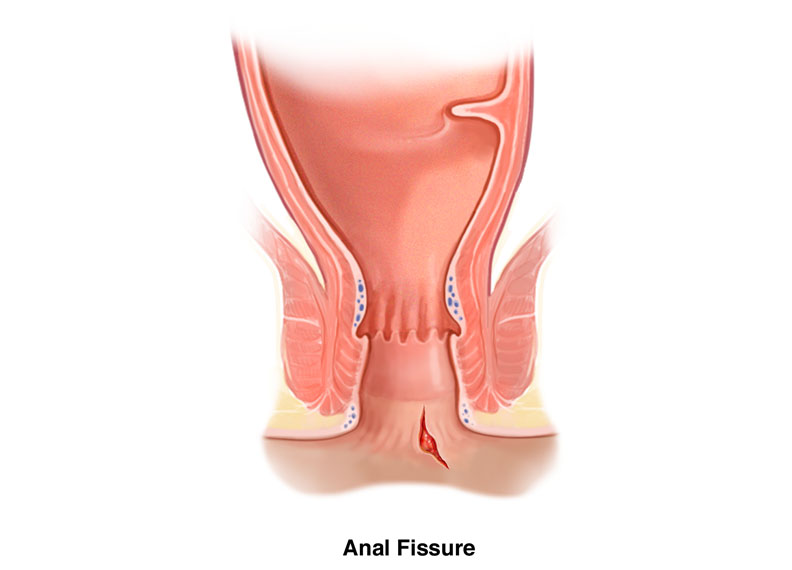
Anal Fissure – Definition
An Anal fissure is a trauma or tear inside the anal canal. It usually causes severe pain or a “burning” sensation, especially when passing stool. Sometimes it is even accompanied by bleeding. Anal fissures can either extend upwards to the lower part of the rectal mucosa or extend downwards, causing the development of swollen skin papilloma on the anal verge, also known as anal papilloma.
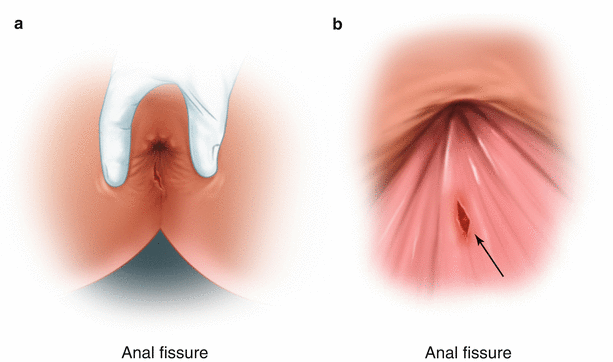
What are the symptoms of an anal fissure?
Usually this injury (tearing) of the anus causes severe pain during defecation and is often accompanied by bleeding and itching. Especially the pain that is triggered during defecation usually lasts for several hours afterwards. The intensity and duration of the pain does not depend on the size of the stretch mark (tear).
Anal fissure is the third most painful condition affecting the anus. The second most painful condition is anal abscess and the first most painful condition is recovery from recent anal surgery.
It is common to have a small amount of blood, which can sometimes mix with the stool.
Quite often, spasm of the anal sphincter muscles, known as anal spasm, can be misdiagnosed as anal fissures. Patients may even undergo surgery. Of course, the pain remains the same after surgery. Moreover, anal fistulas may be mistaken for anal fissures, because it involves an opening in the skin. However, a fissure does not extend into a tract or have an outer opening.
How is anal fissure diagnosed?
The diagnosis of anal fissure is quite easy. A careful overview of the area will often reveal an anal fissure. After mild separation of the skin of the anal verge, the ulcer may be seen. Often the fibers of the muscle of the internal anal sphincter can be seen at the base of this perforated ulcer. (see album). The diagnosis of anal fissure is not made just by the patient describing the symptoms. There is no anal fissure if no tear or ulcer is detected.
The extent of the lesion can be delineated with the help of a finger examination, where the finger is lubricated with a special ointment and a small anoscope. Colonoscopy or examination with a sigmoidoscope helps to rule out abscesses, colitis and other causes of bleeding from the rectum.
An anal fissure must be distinguished from an ulcer, caused by Crohn’s disease, leukemia or malignant tumors, because it has no hairs, is not large and takes a long time to heal. Anal fissures are rarely multiple.